The antiarrhythmic effect is greater when heart rates are slow.įlecainide and propafenone (class IC antiarrhythmic drugs) must be used with an AV blocking drug (beta-blocker or non-dihydropyridine calcium channel blocker) in order to prevent 1:1 conduction of atrial flutter, which can be life-threatening. 
Sotalol exhibits “reverse use-dependence,” meaning at faster heart rates (when potassium channels are being used more), the antiarrhythmic effect is less. Sotalol must be initiated in the inpatient setting in individuals at high risk for QT prolongation to monitor the QT interval and for proarrhythmia. Sotalol has beta-blocker properties, can be used to treat atrial fibrillation and/or ventricular tachycardia, and can prolong the QT interval. Mexiletine is an orally available class 1B antiarrhythmic drug similar to lidocaine and can be used to treat ventricular tachycardia. Lidocaine toxicity can cause seizures and is used intravenously only for the treatment of ventricular arrhythmias. Procainamide and hydralazine can cause drug-induced lupus erythematosus, which can be diagnosed by measuring anti-histone antibodies.ĭisopyramide is used to treat vagally mediated atrial fibrillation and hypertrophic obstructive cardiomyopathy.ĭisopyramide has strong anti-cholinergic properties. Procainamide is used in the setting of Wolff-Parkinson-White syndrome and atrial fibrillation. This results in less toxicity, however, somewhat less efficacy. 
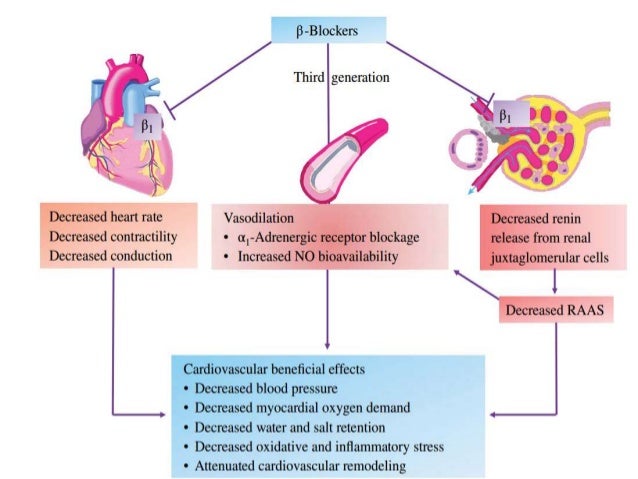
Non-dihydropyridine calcium channel blockers must be used cautiously in patients with systolic heart failure due to their negative inotropic effects.Īmiodarone can cause liver failure (monitor liver function tests), either hyperthyroidism or hypothyroidism (monitor thyroid function tests) and pulmonary fibrosis (monitor pulmonary function tests).Īmiodarone can cause “blue man syndrome,” resulting in bluish discoloration of the skin.Īmiodarone intravenously can cause dramatic hypotension due to the solvents used in the drug preparation.Īmiodarone can cause ocular problems, including sudden blindness on rare occasions.Īmiodarone and dofetilide are the only two antiarrhythmic drugs safe to use in the setting of left ventricular systolic dysfunction.Īmiodarone is only FDA approved for the treatment of ventricular tachycardia and not atrial fibrillation, although it is commonly used for this indication.ĭronedarone is similar to amiodarone, but without the iodine component. The dihydropyridine calcium channel blocker amlodipine has been shown to be safe in the setting of systolic heart failure. ACE inhibitors should be stopped if the creatinine increases to > 2.5 and/or the potassium to > 5.5.ĪCE inhibitors can cause a dry cough thought to be related to the inhibition of bradykinin breakdown (resulting in bradykinin accumulation).Īngiotensin receptor blockers (ARBs) are the preferred drug in patients who are unable to tolerate ACE inhibitors due to a cough. The antidote for beta-blocker overdose is glucagon and inotropes (ie, dobutamine).Īlpha blockers can cause severe first-dose hypotension potentially resulting in syncope thus, alpha blockers are frequently given at night before bedtime.ĪCE inhibitors can cause angioedema, which may be life-threatening, though it is rare.ĪCE inhibitors can cause hyperkalemia and renal failure. Propranolol and metoprolol are lipid soluble beta-blockers and can be used to treat anxiety, migraine headaches, tremor and stage fright. Cardioselective beta-blockers act on beta-1 more than beta-2 and thus will not trigger or worsen asthma as much as non-cardioselective beta-blockers.Ĭarvedilol and labetalol are non-selective beta-blockers that also block alpha-1 receptors.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
